For questions/concerns about this disease in humans, please call your doctor or the Montana Department of Public Health and Human Services (DPHHS).
For questions about this disease/parasite in wildlife, please call the FWP Wildlife Health Lab at 406-577-7882.
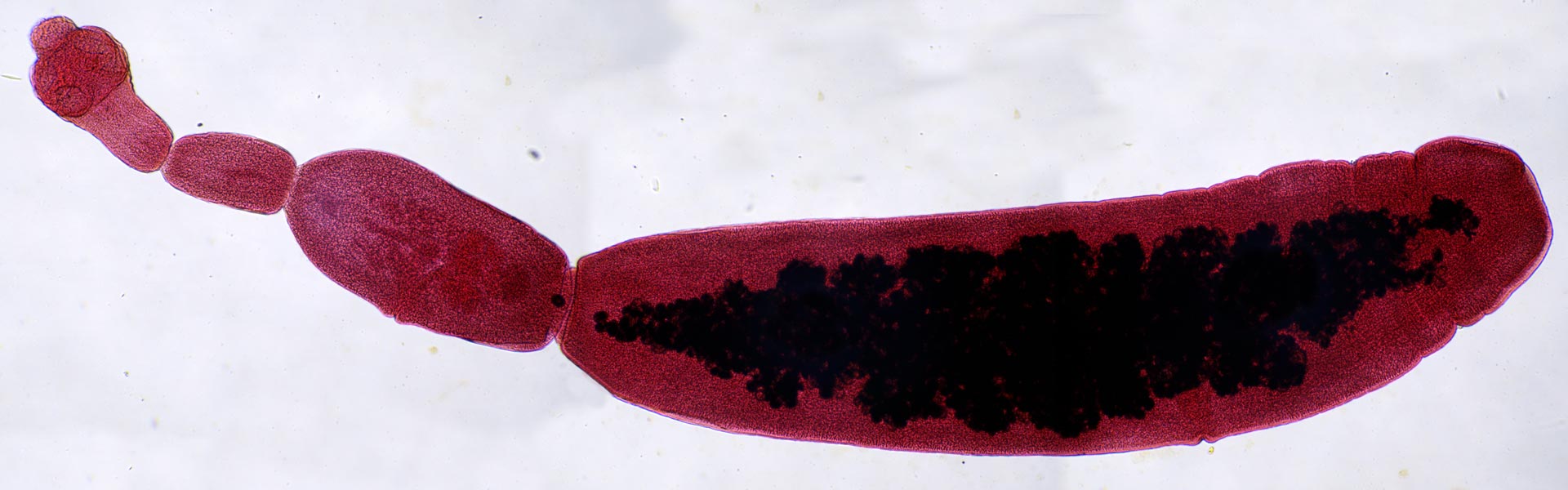
Trichinellosis is a zoonotic (transmissible to humans) parasitic disease of carnivorous mammals and birds caused by infection with the roundworm, Trichinella spiralis. This disease results from the ingestion of larvae of the muscleworm (Trichinella spp.) which is encysted in infected animal tissue. Like other adult roundworms, T. spiralis are un-segmented, cylindrical and tapered at both ends, and can measure 1.2 – 2.2 cm in length (Western, 2009).
Trichinella is present worldwide (except in Antarctica) in domestic and wild animals. In Montana wildlife, Trichinella is present in wild bears and mountain lions. Data are available on the presence of Trichinella in other wild carnivores, but others that could be infected do not generally pose a threat to human health since people do not consume the meat of foxes, coyotes, wolves, and other wild felids.
Trichinosis in wild animals has been studied extensively. At least 22 species of carnivorous mammals and a few predatory birds have been implicated in the transmission of this parasite in North America (Trichinosis, 2007). It is primarily a disease of carnivores with scavenging or cannibalistic tendencies. Wildlife species most commonly infected in North America include bears, coyotes, mountain lions, pigs, raccoons, foxes, wolves, seals and walruses, rodents and mustelids. Humans also can become infected with T. spiralis by consuming undercooked, infected meat (Western, 2009).
Predation and scavenging are thought to be the principal mechanisms by which Trichinella is acquired by animals. Similarly, humans may be infected by eating undercooked or raw meat from an infected animal. Transmission occurs when larvae encysted in the muscle of infected animals is ingested. The larvae are freed from the muscle tissue by the disgestive process and develop into adults in the intestinal tract within four days. Adult female worms produce large numbers of larvae over a short period of time, then die. The new larvae enter the lymphatic system and then the blood stream and are distributed throughout the body where those reaching voluntary mucles encyst. Higher numbers of larvae are found in the most active muscles including the tongue, diaphragm, jaw muscles, and intercostal muscles (between the ribs). Once encysted, the larvae may remain viable for years and are transmitted to the next host when infected muscle tissue is consumed (Davidson 2006). Cysts may remain in muscle for 6-12 months and can survive after death of the host, continuing to serve as a source of infection to scavengers. This nematode has a unique life cycle in which all stages of the parasite occur in a single host (Trichinosis, 2007).
Wild animals rarely show signs of disease (Stitt, 2011). When very large numbers of encysted larvae are present in the muscle, the host animal may experience muscle pain, edema, fever, and rarely, very severe cases may result in death. Unusually large numbers of adult worms in the intestinal tract may result in intestinal hemorrhaging. In bears, a response similar to larval migration in the tissues occurs, but acute disease has not been observed in experimentally infected animals (Trichinosis, 2007).
In humans, the symptoms and duration of disease can vary. Flu-like symptoms such as diarrhea, nausea, vomiting, fever, fatigue and abdominal pain are often early signs of infection. As the disease progresses, patients may suffer from headaches, fevers, chills, cough, swelling of the face and eyes, aching joints and muscle pains, itchy skin, diarrhea, or constipation (CDC). If the infection is heavy, patients may experience difficulty coordinating movements, and have heart and breathing problems. In severe cases, death can occur (CDC).
For mild to moderate infections, most symptoms subside within a few months. Fatigue, weakness, muscle pain, and diarrhea may last for months (CDC).
People can become infected by Trichinella by eating undercooked or raw meat from an infected animal. Infection used to be more common in the United States and was usually the result of consumption of undercooked pork. However, infection is now relatively rare. Human cases decreased beginning in the mid-20th century because of legislation prohibiting the feeding of raw-meat garbage to hogs, commercial and home freezing of pork, and the public education about the danger of eating raw or undercooked pork. Cases are less commonly associated with pork products and more often associated with eating raw or undercooked wild game meats, particularly bear and mountain lion.
People who seek medical treatment for symptoms that are consistent with Trichinella infection should inform their doctor if they consume wild game or undercooked meat. Treatment should begin as soon as possible and the decision to treat is based upon symptoms, exposure to raw or undercooked meat, and laboratory test results (Miller et al, 2003).
All bear and mountain lion meat should be treated as if it is infected. If you eat bear or lion meat, some simple precautions will prevent infection. Thoroughly cook game meat at temperatures of at least 165° F to kill the larvae. Freezing will not kill the organism. Avoid feeding raw or undercooked bear or lion meat to dogs or cats.
Humans may contract Trichinella spiralis from eating improperly cooked meat from an infected animal. Raw or undercooked meat from animals that may be infected should not be fed to dogs or cats. To minimize the chances of infection, meat must be cooked to a temperature of at least 165°F throughout to kill all larvae that may be present. Microwave ovens do not uniformly cook meat and as a result may not kill the parasite. Freezing and curing meat are NOT a reliable way to kill Trichinella roundworms (Trichinosis, 2007). If you harvest an animal and are unsure whether it is safe to eat, contact your local FWP staff for guidance soon after the animal is harvested.
Centers for Disease Control and Prevention (CDC). Website. https://www.cdc.gov/parasites/trichinellosis/index.html
Davidson, William R. 2006. Field manual of wildlife diseases in the Southeastern United States. Athens, Ga: Southeastern Cooperative Wildlife Disease Study, Dept. of population, College of veterinary medicine, The University of Georgia.
Miller, M.J.R., R.D. Dawson, and H. Schwantje. 2003. Manual of Common Diseases and Parasites of Wildlife in Northern British Columbia. University of Northern British Columbia.
Stitt, Tyler. 2011. Diseases You Can Get From Wildlife - A Field-guide for Hunters, Trappers, Anglers and Biologists. British Columbia Ministry of the Environment.
Trichinosis in Montana Bears. 2007. Montana Fish, Wildlife & Parks. Brochure.
Western Wildlife Disease Workshop Notebook. 2009. Southeastern Cooperative Wildlife Disease Study. College of Veterinary Medicine, University of Georgia.
